EVERYTHING YOU NEED TO KNOW ABOUT MELASMA. A Q&A WITH A CONSULTANT DERMATOLOGIST
WHAT IS MELASMA?
Melasma, also known as chloasma, is a common skin condition characterised by skin discolouration, particularly dark patches of skin. Melasma is most commonly found in females, particularly when pregnant, in fact up to 50% of pregnant women experience symptoms, but men can also suffer from this condition. It is also commonly found in women taking hormonal contraceptive pills. Melasma is more common in those with darker skin tones and those who tan very quickly. Melasma is not contagious as it is not an infection so can’t be passed from one person to another, it is also not an indicator of skin cancer or of an allergy.
WHAT ARE THE SYMPTOMS OF MELASMA?
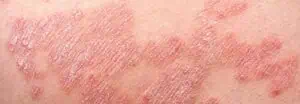
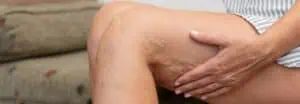
Melasma can appear anywhere on the body which is exposed to the sun. It is most commonly seen on the face, particularly the cheeks, forehead, nose and chin, but is also found on the arms and neck. The areas of melasma will look darker than the surrounding skin and are flat to the skin not raised. Other than appearance, there are no physical symptoms of melasma. The affected skin is not painful or itchy but the condition may cause upset or embarrassment. Symptoms of melasma will become more notable in the summer months in response to sunlight.
WHAT CAUSES MELASMA?
The exact cause of melasma is not fully known. It is thought that the melanocytes in the skin, the pigment producing cells, produce too much pigment in certain areas.
Despite the fact that the cause is unknown, factors which may trigger melasma or make symptoms worsen have been identified. Changes in hormones can trigger melasma which is why it is so commonly seen during pregnancy. The contraceptive pill and other hormone replacements can therefore also be attributed. As with many skin conditions, exposure to UV light in the form of natural sunlight or sunbeds can trigger melasma or worsen symptoms. Melasma is not hereditary, although it is more common in people who have a family history of the condition.
HOW DOES MELASMA DIFFER FROM HYPERPIGMENTATION?
Hyperpigmentation is a term describing increased melanin in the skin giving rise to darker areas. Melasma is a specific type of hyperpigmentation.

HOW IS MELASMA DIAGNOSED?
Melasma is relatively easy to diagnose, and most experienced doctors and dermatologists will be able to diagnose this skin condition by looking at your skin. In rare cases, under local anaesthetic, a small section of skin may need to be removed and examined to eliminate any other skin condition that can resemble melasma.
HOW IS MELASMA TREATED?
There are several ways to treat melasma, both at home and in a medical setting. However, some of these treatments may not be suitable for pregnant women, so it is important to discuss treatment options with a dermatologist.
Firstly, known triggers can be avoided. This can include not taking the contraceptive pill and instead using another form of contraception. Also, avoiding direct sunlight and protecting the skin when exposed to the sun. In milder cases, melasma patches can be covered up using concealers or skin camouflage, a cosmetic cream that is harder to remove. Skin lightening creams can be used which work by preventing pigment cells in the skin from producing melanin. These creams will need to be prescribed by a doctor and you will need to be monitored for any side effects as if misused, they can cause skin damage. Procedures can also be carried out to help treat melasma including chemical peels, microneedling or laser treatments. These treatments work by removing the outer layer of the skin or puncturing this area of the skin which contains the pigment which is needing treating. A consultation with a dermatologist will be required before any treatment takes place to identify which is most suitable.
If your melasma has developed as a result of your pregnancy, symptoms are likely to improve once you have given birth. If your melasma was brought on by pregnancy, you are more likely to see symptoms reoccur during subsequent pregnancies.
HOW CAN MELASMA BE PREVENTED?
As exposure to UV light can trigger melasma or worsen the symptoms, sun protection is very important. Areas of the skin where melasma is present also darkens further in response to sunlight so it is very important to protect your skin in the sun. Wearing sunscreen as well as a face moisturiser of SPF 50 are recommended, as well as covering up when out in the sun and avoiding the strong midday heat. Hormone replacements or the contraceptive pill can also be avoided to prevent melasma symptoms.